
The realization, Drew Starenko said, came while building a home addition by himself in the early 1990s.
He was in his early 30s, he said, and "I was lugging these sheets of plywood up to this roof, and I just kind of stepped back after that and ... said, 'When I'm 50, 55, I don't think I'm going to be able to do this sort of thing.'"
The construction work was never his intended career path, although he'd been doing carpentry since the age of 16.
But if carpentry wasn't a viable long-term occupation, what could he do?
Starenko knew he wanted to work with his hands. He had pre-med and art degrees from Augustana College, and a master of fine arts from the Pratt Institute in Brooklyn.
He had been lured back to the Quad Cities because of some teaching work, but local institutions of higher education weren't hiring full-time art faculty. He had a young family and didn't want to uproot it in pursuit of teaching jobs. And he wanted to stay in the Midwest - which provided much of the inspiration for his art.
So he decided to put his pre-med degree to work - and chose to become a nurse instead of a physician's assistant because it was a quicker path to a job. "I had a daughter and a family," he said.
And nursing, he figured, would also give him time to focus on painting.
From that fundamentally practical choice, a remarkable career began. Starenko is a Certified Registered Nurse First Assistant rather than a surgeon, and he didn't design the equipment or perfect the technique that together make recovery from heart-bypass surgery much easier for patients these days. But he is a local medical pioneer who has directly or indirectly improved hundreds of lives across the globe.
He got his associate's nursing degree in 1995 from Black Hawk College and the next year began working at Genesis Medical Center's east campus. He started in the recovery room, and his locker was next to that of the charge nurse for the cardiovascular unit; in 1997, that nurse asked Starenko if he wanted to join his team.
In 2001, Starenko was the first in the Quad Cities region to perform endoscopic vein harvesting - at the time a relatively new technique used in heart-bypass procedures.
In 2009, he started training doctors and nurses around the world in endoscopic vein harvesting, and he was the first to preform that procedure in Brazil.
And in September of this year, he began working with CardioStart International, an aid organization performing heart surgeries in medically needy parts of the world.
And yes, Starenko is also still an artist.
"I kind of fell into heart surgery," he said. "I really just wanted to be an art teacher and a painter."
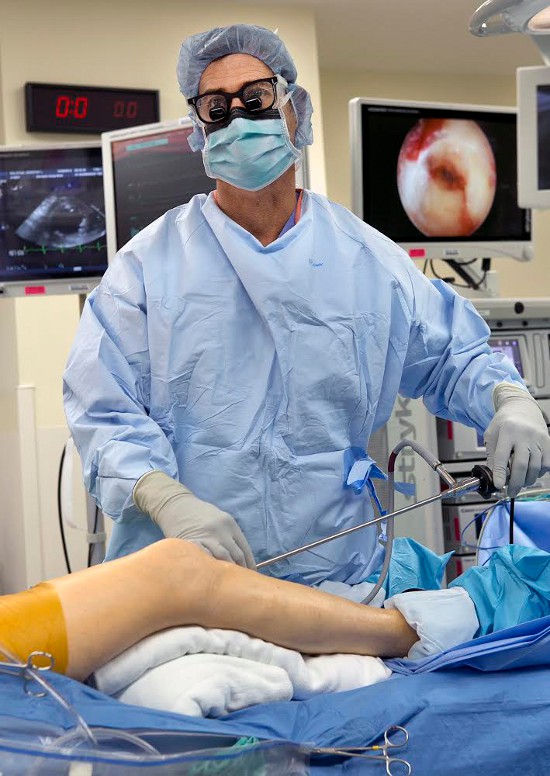
Basic Plumbing
On October 28, there was no indication that the heart-bypass procedure being done in an operating room at Genesis was anything but routine.
The patient was having four grafts, and 10 nurses and doctors would be participating. Music played softly from the room's speakers, and the discussion among the medical personnel ranged from the songs on the radio to the sabbath mode of some ovens.
For the vein-harvesting portion of the surgery, Starenko worked independently of the other medical personnel; his only interaction with other members of the surgery team was asking for sutures. While he was harvesting a saphenous vein from the right leg, a surgeon was opening the chest cavity and harvesting the internal thoracic artery (also known as the internal mammary artery). Starenko would be taking saphenous veins from both legs.
"In a nutshell, it's kind of like basic plumbing in a way, where you have a blockage on a person's artery on the heart and you're taking a conduit from the body and attaching it to a blood supply - which is the aorta - and then routing it past that blockage," Starenko explained.
The mammary artery, he said, is "really the most important graft of the operation. It's to the largest coronary artery." The thoracic artery is also durable, and is likely to stay open far longer than the veins Starenko harvests.
Grafts with the saphenous vein might stay open only 10 to 15 years, he said, because the vein is part of "a low-pressure system, and you're attaching it to the aorta, which is where the pressures are the highest." (Bodies compensate for the removal of the saphenous vein, which is possible because there's an internal blood-flow system that runs near the bones and can do the work in the absence of the superficial removed vein.)
Harvesting the mammary artery is an open procedure, and the surgeon showed me what she was doing. I could see a lung breathing.
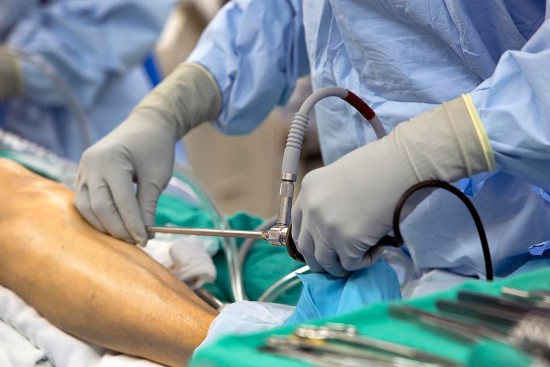
My view of Starenko's work, on the other hand, was largely through a monitor. The endoscope was inserted into the body through an incision - on the inside of the leg below the knee - a few centimeters long, and its camera gave a view of the inside of the body. Starenko's left hand manipulated the endoscopic tools from outside the body, while the right hand appeared to provide finer control of the endoscope itself near the wound. His eyes rarely left the monitor.
After the incision was made, the endoscopic procedure entailed two components.
First, Starenko tunneled around the vein. On the monitor, this looked like so much undifferentiated goo, although Starenko later said I would have been able to see the vein had I known where to look. This portion of the surgery took roughly 25 minutes.
The second component was freeing the vein from its branches - and it was clear from the monitor what was happening. The camera showed a tool that looked like pliers pinching, cutting, and cauterizing the branches, and eventually the vein looked like cable running through a tunnel. After less than 25 minutes doing this, Starenko pulled out roughly 15 inches of worm-like vein still attached to the body at the incision point.
After removing the vein entirely from the body, Starenko began the process of preparing it for grafting - using saline to find leaks from where it had been separated from its branches and repairing them.
Roughly 70 minutes after the initial incision, he was finished with the right-leg saphenous vein.
"Don't Knock Yourself Out, Kid"
Endoscopic vein harvesting such as the procedure I saw is now an unremarkable and common occurrence at hospitals around the United States, but it has taken time for it to become the standard of care for heart-bypass procedures.
"In the old days," Starenko explained, "they would make an incision, depending on how many bypasses a patient was going to have, ... from the groin all the way down to their ankle."
This was a problem for several reasons. First, he said, heart-bypass surgery is already "a huge insult to the body" - and adding another massive wound to the equation made recovery more difficult.
That was exacerbated by the types of patients who typically require bypass surgery. Smoking, diabetes, and obesity, for example, result in "a lot of compromised blood flow to the arms and legs," Starenko said, leading to slow recoveries. "Sometimes, those incisions - as long as they were - would never heal. The infection rate was very, very high, and extremely painful. Patients often complained that their leg incisions were more painful than [recovery from] sawing through their sternum."
For those reasons, he said, doctors and medical-technology companies "were always trying to find methods to not make those large incisions."
Doctors tried, for instance, a "bridging" technique, in which they might make six smaller incisions rather than one large one and tunnel under the skin.
By the late 1990s, companies were marketing equipment for endoscopic vein harvesting, and Starenko was intrigued by the potential: "When this particular technique came out, it just seemed like it was the answer, because it was only done through an incision that was like two centimeters and a teeny little poke up here and a teeny little poke down there depending on how many lengths you needed, and it was all done with inflating it [thus creating a tunnel for better visualization] with CO2 and a scope ... .
"It just seemed to me that it would work. But everybody I talked to [at the hospital] ... said, 'Well, don't knock yourself out, kid, because nobody ... is going to let you do that. ... It's probably going to be a flash in the pan anyway.'"
Still, Starenko attended a training seminar in 2000 in Indianapolis with a company called Guidant (now Maquet), which brought its endoscopic-vein-harvesting equipment to market in 1995.
Genesis, he said, was supportive, but many surgeons were hesitant: "They like new things, but at the same time people are skeptical because we've gone through different things like that before and none of them seemed to work."
The challenge, Starenko said, is the fragility of the tissue used for heart-bypass grafts. "The lining of the vein is only one cell thick that keeps the blood from adhering to the walls," he said. "And so any injury to the vein could compromise the longevity - how long that graft could stay open. ...
"The [endoscopic] surgery was always pretty controversial," he added. "There was always a thought that the endoscopic procedure was more damaging to the vein than doing an open technique." But, he added, "a lot of it is due to the person that's doing the surgery."
After his training, one younger surgeon at Genesis was interested in doing the endoscopic technique for vein harvesting. Other surgeons, he said, still preferred the open method: "We're used to doing it this way. We've always done it this way." Beyond that emotional resistance, Starenko said, many surgeons opted for caution: "Is there more potential for you to compromise the quality of the surgery?"
At the outset, he noted, "the learning curve was very, very steep." Harvesting the veins endoscopically often took longer than doing it the old way.
But the trade-off, Starenko said, was worth it even as he was mastering and becoming more efficient at the endoscopic technique. "You could have it take a little bit longer in the OR [operating room], but there's relatively little complication and very little pain ... in terms of the leg. ... The patients can be up and walking sooner with less pain, ... [which] far outweighs spending a little extra time in the OR."
And new surgeons who came on-board at Genesis, he said, recognized the benefits of endoscopic harvesting and saw it as "the wave of the future."
"A Lifelong Endeavor"
 Starenko has been a part of spreading that wave. In addition to his full-time job at Genesis, he does endoscopic vein harvesting at Trinity and in Iowa City and Peoria.
Starenko has been a part of spreading that wave. In addition to his full-time job at Genesis, he does endoscopic vein harvesting at Trinity and in Iowa City and Peoria.
In 2008, he began doing regional trainings on endoscopic vein harvesting for Maquet. A year later, he became a clinical ambassador for the company and has since done trainings around the world: Finland, Germany, the Netherlands, Turkey, and multiple times in Brazil. (Those trainings are done during his vacation time.)
While the technique is now widely accepted in the U.S., Starenko said he still encounters objections in other countries. Angela Breaux, global training program manager for Maquet, said that roughly 80 percent of heart-bypass procedures in the U.S. now harvest veins endoscopically, but "outside of the U.S., it's pretty much untapped."
In Brazil, Starenko said, "there was still in their minds a controversy" - the concern about potential damage to the vein.
That's often erased, however, when doctors see a patient the next day. "Sometimes they [patients] didn't even know that they'd had an operation on their leg, because the pain was so insignificant," he said.
Breaux said that Starenko is one of several-dozen international trainers Maquet has used. "He's really passionate" about endoscopic vein harvesting, she said. "He's very personable, also. And he adapts to the situation really well."
Doctors in Brazil, she added, "asked for him a few times. And it was because of his being so open - and very nurturing even - in trying to get them to start [with] the new technology."
Starenko is doing fewer Maquet trainings these days, for an obvious reason: As more and more doctors are trained internationally, there's less need for trainers from the United States.
Enter Dr. Emily Farkas, whom Starenko met earlier this year. Farkas is a cardiac surgeon, but for the past eight years she has also volunteered for CardioStart International - an organization that provides free cardiovascular services to medically under-served parts of the world. (It also provides training, equipment, screenings, and medicine to the communities it visits.)
Starenko said he always envisioned himself doing some sort of international medical volunteering, but his career didn't lend itself to it. Heart-bypass operations are expensive and typically done on the elderly, while medical-aid organizations usually focus on lower-cost surgeries for younger patients.
"It's something that I've always wanted to do ever since I got into medicine," Starenko said of volunteering, "and I just didn't quite know what the avenues were that I was going to have to take, because obviously what I do is very specialized."
He thought he might eventually go into public-health work with an organization such as Doctors Without Borders or Partners in Health, but that would have likely required additional training.
When he met Farkas and learned about CardioStart International, however, he saw an opportunity to serve without having to go back to school. "Here's this organization where I can ... do exactly what I know," he said. "This was something I could just jump right into."
And that's what he did. In an e-mail, Farkas wrote that she mentioned to Starenko a September mission to Brazil. "While many clinicians express respect and interest for volunteer work, few take action as expeditiously and decisively as Drew," she wrote. "Within a few days, he had officially applied to be a part of the Brazil team for our mission only a few weeks away."
Starenko said he won't be doing endoscopic vein harvesting with CardioStart, but there's still a need for heart surgery in places without access to good medical care - for example, when strep throat leads to rheumatic fever, which can damage heart valves.
And that's hardly the only need. While in Brazil, Starenko helped treat a seven-year-old boy with "purple lips and gray, ashen fingernail beds, because he had this hole in his heart that was mixing oxygenated blood with unoxygenated blood," he said. "In this country, you would never see a seven-year-old boy like that; that child would have been operated on as a little baby. And here was a seven-year-old kid who had lived like that his entire life."
But because of CardioStart International, Starenko said, "now he will have a normal childhood."
He added that his work with CardioStart will eventually replace his trainings for Maquet - and is "something that I perceive to be a lifelong endeavor." As Farkas asked him: "What else are you in medicine for?"
Volunteer work, he said, is "something that's going to be even closer to me" than endoscopic vein harvesting. Instead of working with medical professionals learning a new technique, he'll be providing direct medical care to people who would otherwise go without it.
His heart patients in the United States, he said, are usually very thankful for the work of their doctors and nurses, but there's an expectation in this country of access to good medical care.
In other parts of the world, he said, the level of gratitude is different: "They hug you, they kiss you - just for taking their blood pressure."
Farkas wrote that Starenko's skills and disposition make him well-suited for the volunteer work he's begun. She listed his "many years of experience and expertise in cardiac surgery" along with "a strong work ethic, a dedication to patient advocacy, and a warm and compassionate spirit. That combination of expertise and empathy is ideal for embracing the complexities of humanitarian work."
She added that she has also seen the artist at work in surgery: "He thinks very carefully about the critical steps of each procedure, yet has the creativity and flexibility to approach each patient and their anatomy individually. Although surgeries are similar, patients are unique. His adaptability, surgical intuition, and elegant problem-solving abilities are valued qualities in any cardiac surgery OR, and crucial in the humanitarian surgery setting, where improvisation and optimal utilization of resources is a reality."

Beauty, Destruction, and Pain
When we first talked for this article in July, Starenko noted some connections between his art background and his medical career.
The endoscopic procedure, he said, is difficult for many medical professionals initially because of the disconnect between the hands and the eyes. In addition, "you're interpreting three-dimensional space on this two-dimensional monitor, which - after teaching it around the world - is not necessarily intuitive ... . It is weird, and it takes a certain amount of getting used to."
But Starenko said his art training made it relatively easy for him to learn and become proficient in the technique. "When I'm just looking at and observing the world, I always see it in terms of a painting. I'm always flattening ... how things look. So you do sort of end up reversing that when you're looking at the monitor [in surgery], because now you're trying to understand the two-dimensional space three-dimensionally."
But in two separate interviews, Starenko said he saw no connection between his medical work and the content of his art. "It's a complete separate thing.," he said. Painting, he added, is "a form of escape from the stresses of the surgery."
Starenko is primarily a landscape artist, and the recent work he showed me was a striking blend of beauty and menace.
One painting is an agrarian landscape dominated by a threatening sky - a pastoral scene overcome by piles of realistic but vividly rendered dark clouds. It has a tension created by the potential for destruction that seems imminent but might end up being a gentle, nourishing shower.
Starenko is also working on a series of charcoal drawings based on satellite photos of hurricanes whose names have been retired - those whose death and destruction have poisoned their common names.
It's clear in the work that the artist is depicting hurricane spirals, but he's abstracted and decontextualized them to the point of geometric elegance. Starenko has captured nature's raw power and balanced it with a sense of awe and wonder - yet also presented those with a detached clarity.
Two days after showing me those works, Starenko e-mailed me a revelation he had while jumping rope - a concise and insightful articulation of the links between the work he does in the operating room and what he does in his downtown-Davenport studio:
"I think the connection simply stated is about life and the fleeting moments that are at once beautiful and at the same time very destructive and painful. Heart surgery is about a second chance oftentimes after a life of abuse and neglect. The surgery itself hovers on this fine line between life and death as we work on the heart, and it is a reminder how fragile we are. I've had a few conversations with surgeons about the beauty and elegance of a surgery, and I find that there is definitely a beauty to it.
"This is also true in my art about the landscape. It is an attempt to show how beautiful it is and at the same time its fragility in how we abuse and pollute it, especially in our industrial agriculture methods. And that there is this fleeting moment when the sun or moonlight hits the clouds and landscape below and for only a moment it's incredible and magic ... and then it's gone."










